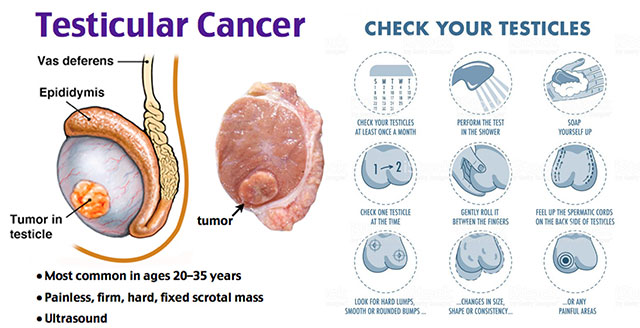
ALTHOUGH testicular cancer is rare, men are advised to make it a point to self-examine their testicles on a monthly basis as a means of detecting early signs of testicular cancer.
According to the Cancer Association of Namibia (CAN) a total of 77 men were diagnosed with testicular cancer between 2007 and 2017 which was recorded on the Namibia National Cancer Registry (NNCR). Most of these cases were recorded in 2017, with 15 men diagnosed. Three deaths from testicular cancer were reported in the same period.
Windhoek-based urologist Dr Hagen Fortsch has urged men to self-examine their testicles. He said testicular self-examination is when a man feels for any changes in consistency and irregularities within the testicles by moving them between his fingers and thumb.
Testicular cancer, which he refers to as a “young man’s” cancer, is common in men between the ages of 15 and 35 and occurs in the testicles (testes), which are located inside the scrotum, a loose bag of skin underneath the penis.
The testicles produce male sex hormones and sperm for reproduction.
Fortsch said it is easier to treat testicular cancer when it is diagnosed early and is highly curable. This is why the doctor believes that self-examination is worthwhile in the early detection of testicular cancer.
“Boys above the age of 15 should monthly self examine under the shower feeling for a hard nodule inside the testicles,” the urologist said.
Fortsch explained that men should feel for any hard lumps that were previously not there, and if they are in doubt, he urged them not to delay visiting a health professional in order to re-examine or do an ultrasound and get treatment initiated immediately.
A normal testicle should not be hard but instead smooth and firm. It is, however, normal for the testicles to be slightly different in size and for one to hang lower than the other.
“But with all cancers, the earlier you detect it, the better the prognosis,” the doctor said. Not all lumps or swellings are cancerous, but anything unusual must be checked by a doctor.
Testicular cancer occurs when healthy sperm cells in a testicle develop abnormalities. “When the sperm production starts there is this massive amount of cell division and if the young man has abnormal chromosomes in one of these sperm cells then they are massively stimulated to divide, and then the cancer can appear,” Fortsch said.
The doctor explained that testicular cancer is not preventable and risk factors such as an undescended testicle is something doctors and men should increasingly be vigilant for.
An undescended testicle is a testicle that is not in the scrotum. A corrective surgery called orchiolysis is done to rectify the positioning of this type of testicle.
“It means that it was in the groin from birth and should have been brought down to the correct anatomical positon by the age of one-and-a-half years, not later,” he stressed.
In order to maintain fertility in men, the surgery should be done by 18 months of baby boy’s life. He said surgery done after this period is too late because the harm is already done to the future life of that testicle, which in turn can affect fertility in a man at a later stage of his life.
If the testes are not there by six months, doctors bring them down by means of orchiolysis surgery. This helps them to easily diagnose testicular cancer if it ever develops in that abnormal testis.
The specialist said every man should know that they have two testicles and parents who see that there is only one testicle should have it investigated.Newborns are always examined for the presence of both testicles.
“There’s no excuse not doing that and if the clinic nurse sees that there’s only one testicle, refer to the next doctor,” he said.
Treatment for testicular cancer ranges from surgery, radiation therapy, and chemotherapy. Even though there is no definitive way to prevent this type of cancer, it is highly curable.
Fortsch said the growth pattern of the cancer determines how treatable this cancer is, adding that the most common type of testicular cancer is seminoma (A cell tumour of the testicle) which is the most eminently treatable.
Having the tumour surgically removed through biopsies is rarely done because this particular treatment increases the risk of the cancer spreading. The tumour is detected through a clinical diagnosis, which includes ultrasounds and blood tests. Doctors will remove the tumour in a process called radical inguinal orchiectomy.
“Men assume that health is a God-given guarantee and heaven forbid that they would have to delegate the responsibility of their health to somebody because they think it’s not masculine,” Fortsch said.
The urologist believes stigma is an inherent barrier for men to get screening and testing, especially when it comes to prostate cancer screening.
“It should not be an issue to carefully permeate your testicles once a month, and make sure that they are safe,” he said, “and if you are in doubt, get professional advice,” he added.
Apart from testicular cancer, men should also be aware of Vanishing Testes Syndrome. A man that only has one testicle should know what happened to the other one.
“That means the testicle was there and then it became suddenly painful and swollen and maybe they got treatment with antibiotics, and then the testicle just simply disappeared,” he said.