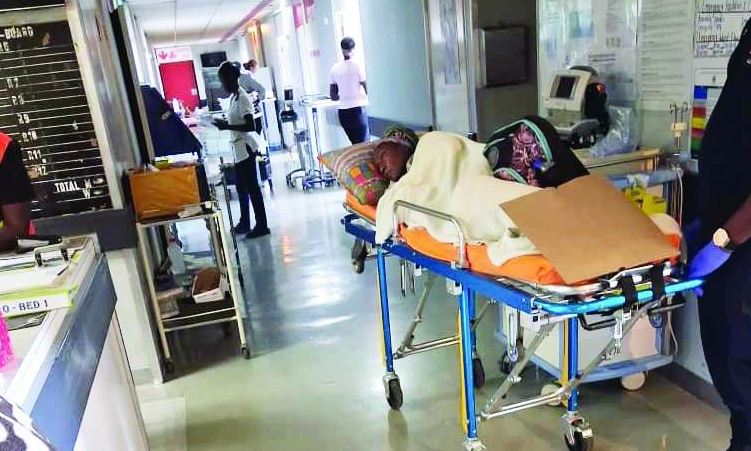
Who Protects Private Healthcare Workers Under Psemas Reforms?

• AMUNYELA SIGFRIED
While the intention to strengthen public healthcare is important, we must also consider the unintended consequences for private healthcare workers.
Private laboratories, medical practices, and private hospitals depend significantly on patient volumes, including Public Service Employee Medical Aid Scheme (Psemas) members, to sustain their services.
If these patients are redirected entirely to public facilities, private labs may experience a sharp decline in test requests and revenue.
This financial strain could result in reduced working hours, hiring freezes, or even the retrenchment of medical laboratory scientists and other healthcare professionals, who are highly trained individuals, playing a vital role in patient diagnosis and care.
At the same time, even if public facilities face increased workloads, the Namibia Institute of Pathology (NIP) may not have sufficient funded posts or budget allocations to absorb medical laboratory professionals who may lose their jobs.
My concern is not to resist reform, but to ask a critical question: As we strengthen public healthcare, who protects the livelihoods of private healthcare workers who have long served this nation?
*Amunyela Sigfried is a medical laboratory scientist at Eenhanha.
Healthcare Reform Must Not Ignore Those Who Contribute

• ALINA-VALENTINA BETUEL
Strengthening and restoring confidence in state healthcare institutions may be the intention, but the debate cannot ignore a fundamental issue: fairness to those who contribute financially every month.
Medical aid contributions are not symbolic. They are deducted consistently from salaries, often at a significant cost, precisely so that members can access healthcare services more efficiently and with fewer delays.
For many families, this is a financial priority. It is money that could have gone elsewhere, but is instead allocated to ensure peace of mind in times of illness.
The expectation is simple: If one is paying for medical aid, one should have reasonable access to private healthcare when needed.
This is not a criticism of Namibia’s public health professionals.
Doctors, nurses, and support staff in public facilities work under demanding conditions. They serve communities across the country, often with limited resources. Their dedication is not in question. What is in question is capacity.
Those who contribute to medical aid do so largely to reduce uncertainty and waiting time. They seek speed, reliability, and choice, especially when health is at stake.
If the government’s goal is to rebuild trust in public healthcare institutions, that objective should be supported. A strong public health system benefits the entire nation, particularly the most vulnerable. However, trust cannot be created through directives alone.
It grows through visible improvements: shorter queues, functioning equipment, adequate staffing, and consistent availability of essential medicines.
There is also a broader question of value. If individuals continue to pay medical aid contributions while facing restrictions on private healthcare access, the perceived benefit of those contributions changes. Transparency and fairness must guide any transition.
Healthcare policy affects real lives. Behind every regulation are parents, workers, pensioners, and children.
Policy decisions must reflect not only national objectives but also the lived experiences of citizens. Namibia deserves a healthcare system that is efficient, equitable, and sustainable.
Reform is necessary, and strengthening public hospitals should be a national priority. But reform must balance collective goals with individual rights and financial commitments.
Healthcare reform must not ignore those who contribute.
If the system is to evolve, it must do so in a way that builds capacity first and preserves fairness throughout the process.
*Alina-Valentina Betuel is an environmental and sustainable development specialist with expertise in land administration and community development.
Equality or Efficiency? Public healthcare reform through Fanon’s ‘zone of being’ and ‘zone of non-being’

• Sakaria Johannes
Access to quality healthcare often becomes a marker of who occupies a privileged space within society.
If government employees previously accessed faster or better medical services, formally or informally, they may have occupied a functional ‘zone of being’ within the healthcare system, while ordinary citizens facing long queues and medicine shortages remained in a ‘zone of non-being’.
By directing government employees into the same public hospitals under the same conditions as everyone else, the state symbolically attempts to collapse this divide and affirm that all Namibians are equal before public services.
From an equality perspective, this initiative carries strong moral weight. When policymakers, teachers, nurses, police officers, and administrators rely on the same healthcare facilities as the broader public, they directly experience the strengths and weaknesses of the system.
Shared experience can generate accountability. It may create political pressure to improve infrastructure, staffing levels, and medicine supply chains.
In this sense, the policy could foster national solidarity and reinforce constitutional ideals of fairness.
Through a Fanonian lens, it appears as an effort to dismantle internal hierarchies within a post-colonial state and to affirm the dignity of all citizens equally.
However, equality within a strained system does not automatically produce efficiency. Public hospitals already struggle with long lines, staff shortages, limited infrastructure, and slow service delivery.
Integrating thousands of additional government employees into an already overburdened system may increase patient volumes without a corresponding increase in capacity.
If no additional doctors, nurses, administrative systems, or medicine supplies accompany this directive, waiting times could grow longer.
Civil servants may spend entire days in queues, which could disrupt operations in schools, ministries, and other public offices.
Teachers absent from classrooms and administrators missing from their posts due to extended hospital visits could indirectly affect service delivery across the country.
In attempting to create equality in healthcare access, the state may inadvertently shift inefficiencies into other sectors.
- Sakaria Johannes is a political science graduate from the University of Namibia. He can be reached at sackyuutsi@gmail.com
In an age of information overload, Sunrise is The Namibian’s morning briefing, delivered at 6h00 from Monday to Friday. It offers a curated rundown of the most important stories from the past 24 hours – occasionally with a light, witty touch. It’s an essential way to stay informed. Subscribe and join our newsletter community.

The Namibian uses AI tools to assist with improved quality, accuracy and efficiency, while maintaining editorial oversight and journalistic integrity.
Stay informed with The Namibian – your source for credible journalism. Get in-depth reporting and opinions for
only N$85 a month. Invest in journalism, invest in democracy –
Subscribe Now!